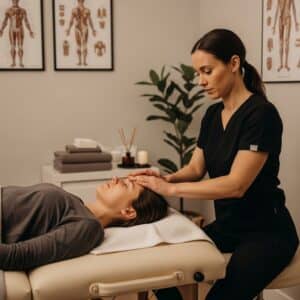
Craniosacral Massage Therapy
Craniosacral massage therapy is a subtle form of bodywork that focuses on the relationship between the nervous system, connective tissue, and the physical structures of the body. While often described in abstract or overly complex terms, its practical function is straightforward. It works by reducing tension within the system that surrounds and protects the brain and spinal cord, while influencing how the body regulates stress and recovery.
This approach differs from traditional massage techniques that rely on pressure and mechanical manipulation. Instead, craniosacral work uses very light contact to interact with deeper patterns of restriction. These patterns are often not purely muscular. They are tied to how the body holds tension over time through posture, stress, and compensation.
Understanding the Craniosacral System
The craniosacral system includes the membranes and fluid that surround the brain and spinal cord, extending from the head down through the sacrum. This system is closely connected to the nervous system, which controls how the body responds to stress, pain, and environmental input. When tension develops within this system, it can influence both physical and neurological function.
Restrictions may develop from injury, repetitive strain, prolonged stress, or long-term postural imbalance. These restrictions do not always present as obvious pain. In many cases, they show up as subtle dysfunction such as persistent tightness, fatigue, reduced mobility, or a constant feeling of tension that does not fully resolve.
How Craniosacral Massage Therapy Works
Craniosacral massage therapy works through slow, controlled contact that allows the body to shift out of a guarded state. The nervous system plays a central role in this process. When the body perceives pressure or force, it often responds by resisting. When contact is minimal and steady, the system is more likely to relax and release tension on its own.
This shift allows deeper layers of the body to respond without force. Tissue begins to soften, movement improves, and areas of restriction can be addressed indirectly. The process is not immediate or aggressive. It builds gradually as the body recognizes that it no longer needs to maintain the same level of tension.
Nervous System Regulation and Stress Response
One of the primary effects of craniosacral massage therapy is its influence on the nervous system. Chronic stress keeps the body in a heightened state of alertness, which maintains muscular tension and limits recovery. Over time, this becomes the baseline condition for many individuals.
By working with the body in a non-invasive way, craniosacral therapy helps shift the nervous system toward a more regulated state. Breathing slows, muscle tone decreases, and the body begins to move away from constant activation. This change allows for deeper recovery and improved overall function.
Connection to Muscular and Fascial Tension
Although craniosacral therapy does not rely on deep pressure, it still affects muscular and fascial structures. The body is connected through a continuous network of connective tissue that links distant regions together. Tension in one area can influence movement and comfort in another.
By reducing restriction within the craniosacral system, the body can reorganize how tension is distributed. Muscles that were previously overactive may begin to release, while underused areas can engage more effectively. This creates a more balanced and efficient pattern of movement.
When Craniosacral Massage Therapy Is Used
Craniosacral massage therapy is often used when traditional approaches have provided limited or temporary relief. This includes situations involving chronic tension, stress-related discomfort, headaches, and persistent patterns that do not respond to direct pressure alone.
It is also used as a complement to more active forms of massage therapy. While deeper work addresses muscular restriction directly, craniosacral techniques can support the nervous system and help maintain those changes between sessions.
Consistency and Adaptation
Like all forms of bodywork, craniosacral therapy produces better results when applied consistently. The body adapts over time. Subtle changes accumulate, leading to more stable improvements in comfort and function. This is especially important for individuals dealing with long-standing patterns of tension or stress.
Repeated sessions allow the nervous system to recognize a new baseline. Instead of returning to a state of constant tension, the body begins to maintain a more relaxed and balanced condition. This reduces the frequency and intensity of discomfort over time.
Craniosacral Massage Therapy in Olympia, WA
Craniosacral massage therapy offers a different approach to addressing tension and dysfunction. Rather than forcing change through pressure, it works with the body’s existing patterns, allowing them to release in a controlled and sustainable way.
For those seeking craniosacral massage therapy in Olympia, WA, this method can be used as part of a broader massage therapy approach focused on reducing tension, improving recovery, and supporting long-term physical function.
